Month: August 2019
-

Exploring the Potential Impact of Genetics and Infection on T1D Risk
There is no clear, concise explanation for why some people develop type 1 diabetes (T1D) and others do not, or what puts some people at greater risk for the disease. […]
-
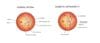
Asthma Medication May Help Treat Diabetic Retinopathy
A common complication associated with diabetes (T1D) is diabetic retinopathy. Poor blood sugar control can increase risk of this disease because it impacts the blood flow to the eye by […]
-

Structured Mealtime Routines May Help Manage HbA1c Levels in Young Children with Type 1 Diabetes
Managing type 1 diabetes (T1D) can be challenging for anyone, but it can be especially difficult for parents of young children with the disease. They must carefully monitor their child’s […]
-

Nasal Glucagon Approved to Treat Severe Hypoglycemia
If you or someone you love is living with type 1 diabetes, you know that, in addition to blood sugar becoming too high, having it drop too low is a […]
