Month: December 2017
-

2017 Year in Review
This past year has been a year of impact at the Diabetes Research Connection. With the generosity of our supporters, we funded five innovative, peer-reviewed type 1 diabetes (T1D) projects, […]
-
Stem-Cell Derived Therapy for Type 1 Diabetes Funded to Move Forward
Scientists have been exploring many options for treating and potentially curing type 1 diabetes (T1D) in recent years. From examining the role of gut cells to creating an artificial pancreas, […]
-
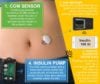
How Technology is Changing Diabetes Care and Treatment
Despite years of research and clinical trials, no cure for type 1 diabetes exists yet. However, how the disease is managed and treated has changed, leading to vast improvements in […]
-
Could There be More than two Types of Diabetes?
Could There be More than Two Types of Diabetes? Diabetes is a metabolic disease that, according to common knowledge, is classified into two main types. However, recent studies suggest the […]
-

Could Blood Stem Cells Be Used to Reverse Type 1 Diabetes?
Researchers know that in individuals with type 1 diabetes, the body mistakenly attacks and destroys insulin-producing beta cells that are used to regulate blood sugar levels. One of the challenges […]
-
Potential Benefits of Incorporating Metformin in Type 1 Diabetes Treatment
Traditionally metformin is a drug used to help control blood sugar in individuals with type 2 diabetes. However, a recent study examined its effects in patients with type 1 diabetes. […]
-
Treating Type 1 Diabetes with Synthetic Cells
Treating type 1 diabetes (T1D) takes careful planning and calculation. Individuals must test their blood to determine their blood glucose level, then calculate exactly how much insulin they need to […]
-
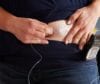
Comparing Insulin Pumps and Injections for Managing Type 1 Diabetes
Learning how to effectively manage type 1 diabetes can take time. It takes practice and trial-and-error to understand how each person’s body responds to different foods, activities, and insulin doses. […]
-
New Biomarker May Help with T1D Detection, Prevention, and Treatment
As scientists continue studying type 1 diabetes (T1D), they develop a deeper understanding of changes that occur in the body. It has been known for a while that the body […]
