Month: February 2021
-

Discussing Diabetes with DRC’s T1Ds: Blog Post 4
As a type 1 diabetic who considers the beach their second home, I can say that Beyond Type 1’s “T1D Beach Guide” is spot-on. While splashing in the waves or […]
-
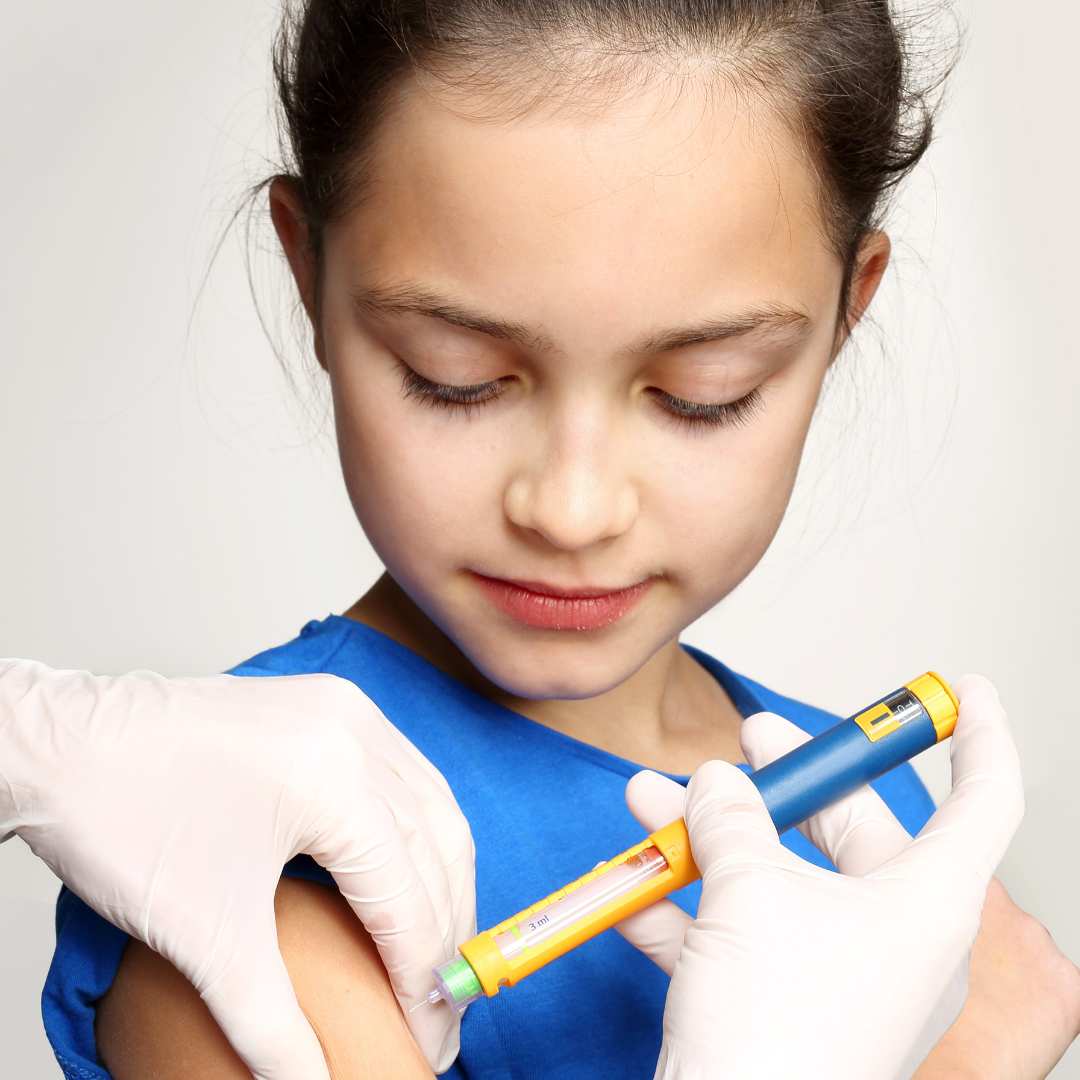
New Guidelines Lower Target HbA1C Levels for Children with Type 1 Diabetes
One of the goals in managing type 1 diabetes is reducing fluctuations in blood glucose levels. Maintaining a stable blood sugar is ideal, which means consistently monitoring glucose levels and […]
-

DRCs 1st Virtual Gathering of 2021!
On Tuesday, February 23, DRC held it’s first virtual gathering of the year. DRC partnered with the Chris Dudley Foundation for a Meet and Greet, where Chris Dudley shared his […]
-

Discussing Diabetes with DRC’s T1Ds: Blog Post 3
When I responded to the article, “10 Ways the Pandemic Parallels “Normal” Chronic Illness Life,” it mentioned “bleak burnout,” which I stated that I resonated with. This week, I decided […]
-

Coronavirus and Diabetes Resources: Community Partner with Beyond Type 1
It is no secret that this pandemic has made life extremely more challenging. And for those with type one diabetes (T1D), infinitely more so. Fortunately, Beyond Type 1, a nonprofit organization […]
-

Discussing Diabetes with DRC’s T1Ds: Blog Post 2
Finger-pricking, insulin dosing, tracking food consumption, monitoring glucose levels: type 1 diabetes is a mentally and physically taxing full-time job. As a type 1 diabetic myself, I know how quickly […]
-

Pushing for Improved Prioritization for COVID-19 Vaccine for Individuals with Type 1 Diabetes
As the United States has begun rolling out COVID-19 vaccines across the country, it has also created guidelines regarding eligibility and prioritization for the drug. There are multiple phases with […]
-
First Generic Glucagon Approved by FDA to Treat Severe Hypoglycemia
A significant concern for individuals with type 1 diabetes (T1D) is preventing severe hypoglycemia, also known as very low blood sugar. When blood glucose levels drop too low, it can […]
-

Disordered Eating May Increase High Blood Sugar Risks in Type 1 Diabetes
Type 1 diabetes (T1D) can be a difficult condition to manage. Individuals must continuously be aware of their food and beverage intake, physical activity, overall health, and how this impacts […]
-

Could Eating Fish Help Prevent Type 1 Diabetes?
Although type 1 diabetes often develops in childhood, that is not always the case. In some instances, the disease may not fully develop until adulthood. The body may produce autoantibodies, […]
-

Double Trouble: Managing Type 1 Diabetes & Celiac Disease
As anyone with type 1 diabetes (T1D) knows, managing life with an autoimmune disorder can be challenging. Individuals with T1D must be regularly monitoring their blood sugar, adjusting insulin based […]
-

Discussing Diabetes with DRC’s T1Ds: Blog Post 1
*DRC will begin a new campaign where those with type one diabetes (T1D) in the DRC community will share their thoughts and personal anecdotes in response to lifestyle articles related […]
