Month: May 2019
-

Researchers Improve Cell Conversion to Support Diabetes Treatment
One of the methods of treating type 1 diabetes that researchers have been exploring is using patients’ own cells. They found that by converting stem cells into insulin-producing beta cells […]
-

Enteroviruses May Be Linked to Higher Type 1 Diabetes Risk
As with many diseases, type 1 diabetes is triggered by both genetic and environmental factors. There is not a single cause that can be pinpointed when it comes to why […]
-
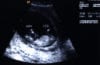
HbA1c Levels May Influence Preterm Birth Risk
Maintaining healthy HbA1c levels is essential for individuals with type 1 diabetes (T1D), but it may be especially critical for women seeking to have children. A recent study out of […]
