Month: November 2015
-

KUSI Good Morning San Diego Interviews DRC’s Very Own Alberto Hayek
Introduction to the KUSI Good Morning San Diego Interview with DRC Local television programming can often give us insights and connections to our community that other media simply can’t. One […]
-
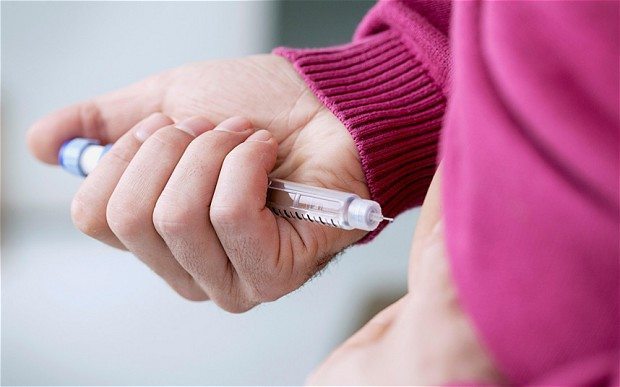
End of Daily Injections for Diabetes as Scientists Restore Insulin Production
Original article written by Sarah Knapto, Science Editor, for The Telegraph on November 25, 2015. Click here to read the original article. The end of daily injections for diabetes sufferers […]
-

Connecting Donors Directly to Researchers
The Diabetes Research Connection connects donors with early-career scientists enabling them to perform peer-reviewed, novel research designed to prevent and cure type 1 diabetes, minimize its complications and improve the quality of life for those living with the disease.
